UnitedHealth Group’s decision to cut prior authorization requirements by 30% may sound like a technical adjustment, but it targets one of the most widely criticized mechanisms in U.S. healthcare. According to a The Wall Street Journal report, the move is intended to simplify access to a range of routine services, including certain diagnostic tests, outpatient procedures, and therapy approvals.
Prior authorization is the process insurers use to approve certain tests, treatments, or procedures before they are performed. In theory, it helps control unnecessary spending. In practice, it often creates delays and adds complexity. Data shows that nearly half of patients who went through prior authorization describe the process as difficult to navigate, according to a Kaiser Family Foundation analysis.
The scale of how often patients encounter this system is larger than many assume. About 51% of insured adults say they have been required to obtain prior authorization for treatment, medication, or services within the past two years. That means the process is not an edge case - it is a routine part of healthcare access.
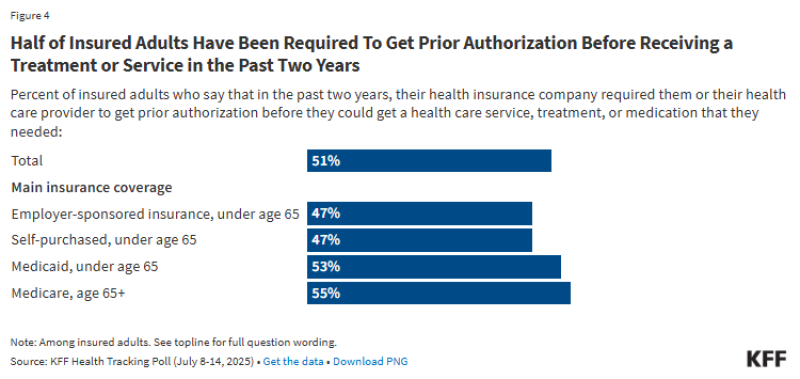
When more than half of patients go through the same approval process, even small changes can affect millions of care decisions. That widespread exposure helps explain why the issue has become so visible. Surveys show that 73% of Americans consider delays and denials by insurers to be a major problem, with similar levels of concern across income groups, political affiliations, and insurance types.
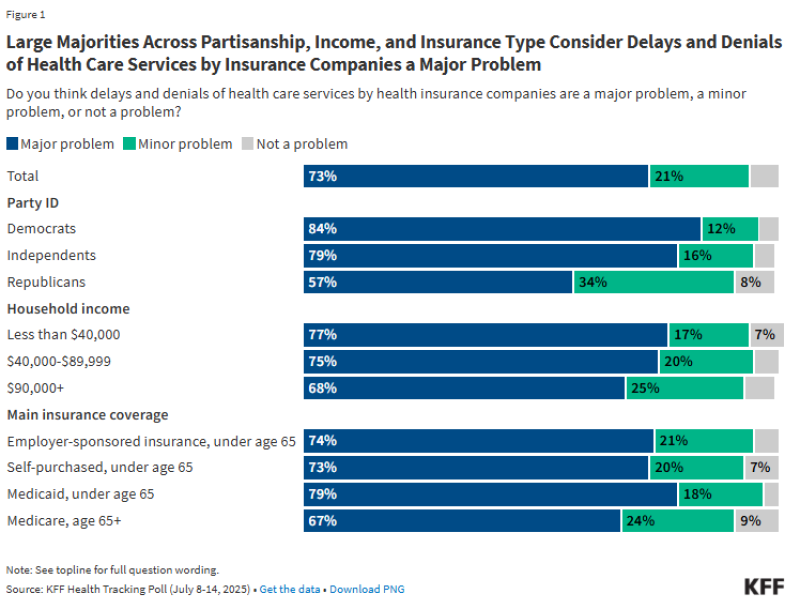
The concern is not just about inconvenience - it reflects real consequences. Around 29% of insured adults report that their care was delayed or denied by their insurance company in the past two years. Breaking that down further, 24% experienced delays, while 22% reported outright denials, indicating that the system can directly affect whether and when patients receive treatment.
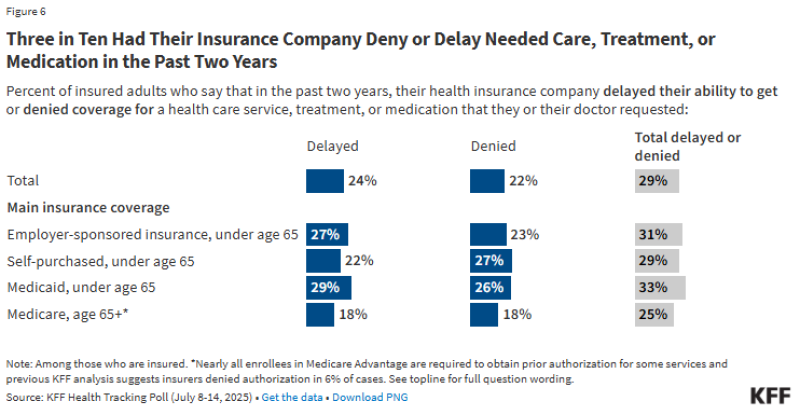
The burden is not limited to patients. Physicians have long criticized prior authorization for the time and complexity it adds to care delivery. Surveys from the American Medical Association show that doctors spend substantial time each week managing approval requests, often delaying treatment decisions and diverting resources away from patients.
This is the context in which UnitedHealth’s decision should be understood. By reducing authorization requirements, the company is effectively removing a layer of friction from a process that affects a majority of patients and is widely viewed as problematic.
For patients, this could translate into faster access to tests, surgeries, and therapies. For providers, it reduces administrative overhead and allows more decisions to be made at the point of care.
At the same time, the system is not being eliminated. Prior authorization will still apply to more complex or high-cost procedures, suggesting that insurers are attempting to rebalance rather than abandon cost controls altogether.
Insurers argue that prior authorization plays a critical role in preventing unnecessary or overly expensive treatments. Without it, they warn, healthcare utilization could rise, putting upward pressure on premiums.
 Marina Lyubimova
Marina Lyubimova

 Marina Lyubimova
Marina Lyubimova


